Does Insurance Cover Cosmetic Dentistry: What’s Covered?
If you're looking in the mirror and thinking about veneers, Invisalign, implants, or brighter teeth, the biggest question usually isn't whether the result would look good. It's whether insurance will help pay for it.
For many patients in Las Vegas, that question gets frustrating fast. One person hears whitening isn't covered. Another is told a crown might be. Someone else gets partial coverage for aligners after a long review. That's why the honest answer to does insurance cover cosmetic dentistry isn't a simple yes or no. It depends on why the treatment is being done, how it's coded, and what documentation goes to your plan.
At a practical level, dental insurance usually covers care that protects health or restores function. It usually does not cover treatment done only to improve appearance. The challenge is that some of the most popular smile treatments sit right in the middle.
Cosmetic Dentist in Las Vegas Explains Dental Insurance
A lot of people start in the same place. They want a better smile, but they don't want to commit to treatment until they understand the cost. That's smart.

In the United States, standard dental plans usually exclude purely cosmetic work. The American Dental Association reports that 63% of adults have private dental benefits, but those benefits are mainly built around preventive, basic, and major restorative services rather than elective aesthetic treatment. The same ADA overview also notes that Americans spend billions annually on cosmetic work out of pocket because coverage is limited for services such as whitening and similar elective procedures (ADA dental coverage and access overview).
Why patients get mixed answers
Insurance companies don't make decisions based on whether a treatment sounds cosmetic. They make decisions based on how the procedure is classified and whether the record shows a health or function problem.
That means two treatments that improve appearance can be handled very differently. A front tooth crown placed because the tooth is broken may qualify for benefits. Veneers placed only to brighten a smile usually won't.
Practical rule: If a procedure repairs damage, protects a tooth, restores chewing, or addresses pain, it has a much better chance of being considered for coverage.
The answer is usually no, but not always
Many patients feel stuck in this situation. They hear "cosmetic isn't covered" and assume every smile treatment is self-pay.
That isn't always true. Some services fall into a gray area, especially when they also support oral health. Before making assumptions, it helps to understand how dental insurance works and what your specific plan calls medically necessary care.
For patients searching for a cosmetic dentist near me or a dentist in Las Vegas, NV, the best first step is a consultation that looks at both the smile goal and the insurance angle. That's often the difference between a flat denial and partial coverage.
Defining Cosmetic vs Medically Necessary Dentistry
Think of dental insurance like auto insurance. It will usually help pay to repair collision damage. It usually won't pay to add custom styling just because you prefer the look.
Dental plans work in a similar way. They tend to cover treatment that restores health, structure, or function. They tend to exclude treatment that's done only to improve appearance.
How insurers make the distinction
Dental insurance relies on Current Dental Terminology, or CDT, codes. These codes tell the insurer what procedure was performed and help determine how the claim is processed. According to Delta Dental's explanation of cosmetic classification, purely cosmetic treatments such as teeth whitening codes D9971 to D9975 and aesthetic porcelain veneers D2960 to D2962 are typically excluded with 0% coverage. The same source notes that a crown on a decayed tooth, such as D2740, can qualify for up to 50% coverage as a major restorative service when it's documented as medically necessary.
That coding step is why a dentist's notes matter so much. The insurer isn't just looking at the final result. It's looking at the reason behind it.
Cosmetic vs restorative dental procedures at a glance
| Procedure | Typically Cosmetic (Often Not Covered) | Typically Restorative (Often Covered) | Can Be Either (Coverage Depends on Proof of Need) |
|---|---|---|---|
| Professional teeth whitening | Yes | ||
| Filling for decay | Yes | ||
| Crown | Yes | Yes | |
| Veneers | Yes | Yes | |
| Bonding | Yes | ||
| Invisalign or clear aligners | Yes | ||
| Dental implants | Yes |
A simple way to read this table is to ask one question. Is the main purpose appearance, or is the treatment also fixing a real problem?
If you're comparing smile options and want a general consumer-friendly overview, this discussion of cosmetic smile enhancements at The Smile Spot is a useful companion resource. It helps frame why some procedures are chosen purely for aesthetics while others overlap with function.
A treatment can look cosmetic and still qualify as restorative if the clinical reason is strong enough.
What that means in real life
A veneer placed because you want a whiter, more uniform smile is usually cosmetic. A similar restoration placed to protect a damaged tooth may be reviewed differently. A crown on a weak tooth may improve appearance, but insurance is focused on the protection and function it provides.
This distinction matters whether you're booking a smile consultation, replacing a missing tooth, or looking for dental implants near me. It also matters when patients are deciding between cosmetic dentistry and restorative dentistry, because the insurance outcome may be very different even when the two options look similar.
Procedures Insurance Almost Always Excludes
Some treatments are straightforward from an insurance standpoint. If the service is done only to improve appearance, standard dental coverage usually won't pay for it.
Whitening and appearance-only veneers
Professional teeth whitening is one of the clearest examples. Whether a patient wants in-office whitening for photos, a wedding, or just a fresher look, insurers usually see it as elective because it doesn't treat disease or restore function.
Veneers can fall into the same category when they're used only to change color, shape, or minor spacing. If healthy teeth are being cosmetically enhanced, insurance usually treats that as a personal choice rather than a covered dental need.
Other elective aesthetic procedures
Patients are often surprised by these exclusions because the treatments are still provided by a dentist. But insurance isn't asking who performs the service. It's asking whether the service is medically necessary.
Common examples that are often excluded include:
- Smile brightening only: Whitening intended only to improve tooth color.
- Shape refinement: Veneers or bonding placed only to alter contour or symmetry.
- Cosmetic gum contouring: Reshaping gum tissue when there's no functional or periodontal reason.
- Minor appearance upgrades: Replacing acceptable restorations only because they don't match the look you want.
For Las Vegas patients, expectations need to be realistic. If the treatment goal is purely aesthetic, it's better to plan for self-pay, financing, or a membership discount instead of expecting a claim check later.
Insurance usually says no when the problem is cosmetic preference rather than pain, damage, decay, or impaired function.
That's not meant to discourage anyone from improving their smile. It helps avoid the frustration of assuming a plan will reimburse a treatment it was never designed to cover.
When Cosmetic Dentistry May Be Covered by Insurance
The gray area is where most of the actual questions live. Some procedures improve the look of a smile and also solve a functional problem. That's when coverage becomes possible.
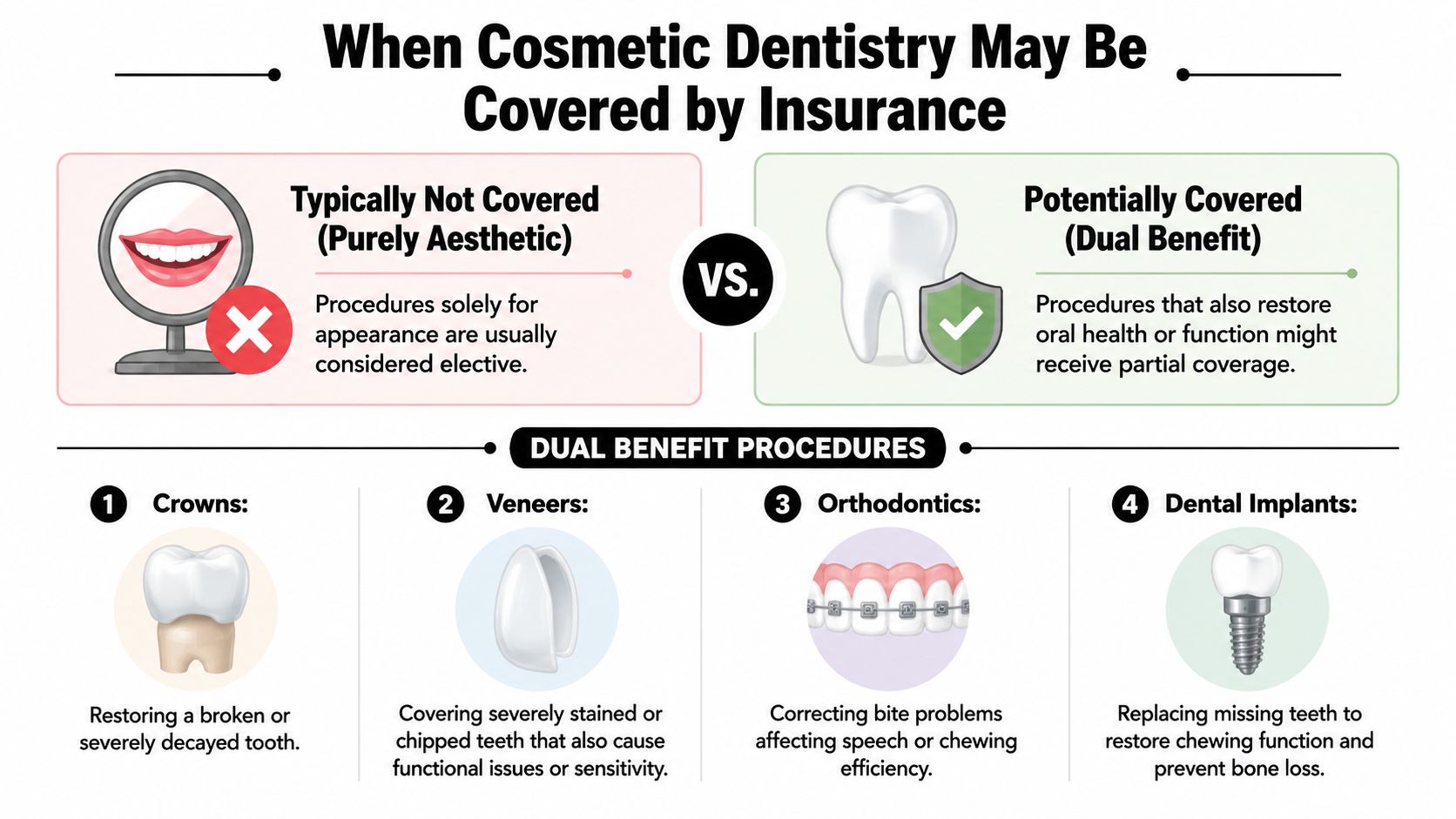
Clear aligners and bite problems
Clear aligners are a good example. Adults usually don't get broad orthodontic coverage just because they want straighter teeth. But this review of cosmetic dentistry insurance rules notes that adult coverage for clear aligners is rare, yet it may be partially covered up to 50% with lifetime caps of $1,500 to $3,500 when severe malocclusion causes functional problems.
That matters if crooked teeth are contributing to uneven wear, chewing difficulty, or related jaw strain. In that case, the issue isn't just cosmetic. It's structural.
Implants, crowns, and dual-purpose treatment
The same source explains that dental implants are increasingly covered at 30% to 50% in employer plans when they're justified as necessary to restore function and help prevent bone loss after extraction. That's a major distinction for patients searching for dental implants near me after losing a tooth.
A few common examples help show how this works:
- Broken front tooth: A crown may improve appearance, but if the tooth is structurally compromised, insurance may view it as major restorative care.
- Missing tooth: An implant might make the smile look complete again, but it also supports chewing and helps maintain oral function.
- Severe bite issues: Invisalign may be reviewed more favorably when the records show functional problems, not just crowding or aesthetics.
- Damaged enamel or trauma: In select situations, a veneer or similar restoration can move out of the purely cosmetic category if it protects the tooth.
Documentation is what changes the outcome
This is the part many people miss. Coverage doesn't depend only on the procedure name. It depends on what the clinical record proves.
Useful documentation often includes:
- Diagnostic images such as dental x-rays or other scans.
- A written narrative explaining pain, fracture, wear, missing structure, or chewing limitations.
- Correct CDT coding so the insurer understands the restorative reason for treatment.
- Pre-authorization before treatment begins, especially for borderline cases.
A beautiful result doesn't disqualify treatment from coverage. Lack of documented medical necessity usually does.
For patients in Las Vegas who need cosmetic dentistry with a restorative component, the strongest cases are built before treatment starts, not after a denial arrives.
How to Confirm Your Specific Dental Coverage
General rules are helpful, but your plan decides what you pay. The fastest way to avoid surprises is to verify benefits before treatment begins.

Start with a pre-treatment estimate
Ask the dental office to submit a pre-treatment estimate or pre-authorization whenever a procedure might fall into that cosmetic-restorative gray area. That gives the insurer a chance to review the code, images, and clinical notes before you move forward.
If you're trying to sort through plans or find a local office that can help with that process, this guide on how to find a dentist that accepts my insurance is a practical place to start.
Questions worth asking your insurance company
Don't call and ask only, "Do you cover veneers?" That's usually too broad to get a useful answer. Ask more specific questions.
Use a short checklist:
- Procedure details: Ask whether the exact CDT code is covered under your plan.
- Medical necessity rules: Ask what documentation is required for review.
- Waiting periods: Confirm whether major services have a delay before benefits apply.
- Annual maximums: Ask how much benefit remains for the current year.
- Deductible and coinsurance: Find out what portion you would still owe if coverage is approved.
- Pre-authorization requirements: Ask whether approval is required before treatment begins.
- Appeals process: Request the steps if the initial claim is denied.
Let the office send the right paperwork
A good claim submission usually includes more than a code. It may need x-rays, chart notes, a narrative, and a clear explanation of why the treatment restores health or function.
This overview gives a simple visual explanation of how the insurance review process works:
If a claim is denied, don't assume it's over
Denials happen for many reasons. Sometimes the insurer needs more documentation. Sometimes the original submission didn't clearly show the functional problem. Sometimes the plan exclusion is real.
When an appeal makes sense, stay organized. Keep the estimate, denial notice, radiographs, and supporting notes together. A cleaner record gives you a better shot than a rushed follow-up.
Affordable Alternatives for Your Dream Smile
If insurance won't cover the treatment you want, that doesn't mean the conversation ends there. It just shifts from insurance strategy to payment strategy.
Membership plans can close the gap
One of the most practical workarounds is an in-house dental membership plan. According to Delta Dental Connecticut's discussion of cosmetic dentistry coverage, dental membership programs have grown 42% in the U.S. and commonly offer 20% to 50% discounts on services like veneers or implants for a flat annual fee. That source also notes the trend is especially relevant in Nevada, where demand for cosmetic treatment is high.
For patients paying out of pocket, that structure can be easier to understand than traditional insurance. There are no claim surprises for excluded cosmetic treatment because the discount is usually built into the plan terms from the start.
Other ways patients make treatment manageable
Different payment tools work for different cases. A smaller whitening case may need a simple monthly arrangement. A larger implant or smile makeover plan may need phased treatment.
Common options include:
- FSA or HSA funds: These can help with qualifying dental expenses when allowed under your plan rules.
- Monthly financing: Third-party healthcare financing can spread larger treatment costs over time.
- Phased care: Treatment can sometimes be sequenced so urgent or restorative steps happen first.
- Practice membership discounts: These may reduce costs on services that insurance excludes.
If you're trying to compare approaches before committing, this overview of options for dental care without insurance offers a useful outside perspective on how patients handle treatment costs when standard coverage falls short.
The most affordable plan isn't always the one with the lowest sticker price. It's the one you can actually complete without stopping halfway through care.
In Las Vegas, many families also combine routine preventive care with a membership arrangement and then use financing for elective smile upgrades. That kind of blended approach often works better than waiting for insurance to approve something it was never built to cover.
Your Partners in Cosmetic Dentistry in Las Vegas
For patients in Las Vegas, the most important part of this process is getting a treatment plan that makes sense clinically and financially. That means looking at the smile goal, checking whether any part of the case can be documented as medically necessary, and then mapping out the remaining balance clearly.
Nevada adds an important practical angle. According to this discussion of Nevada cosmetic dentistry coverage, plans in the state are required to cover medically necessary major procedures such as crowns and implants at around 50%, while purely elective cosmetic work is excluded. The same source says a 2025 Nevada Division of Insurance report found 68% of claims for hybrid cosmetic-restorative work were approved when strong dentist documentation was included. That's why pre-authorization matters so much for cases that sit in the middle.
What patients can expect locally
At Aspiring Smiles Dental and Braces, patients can come in for a consultation, review treatment options, and have the office help check benefits before moving forward. That can be useful for people considering Invisalign, crowns, implants, veneers, or professional whitening and trying to compare what's insurance-eligible versus what would be paid out of pocket.
The office is located at 3211 N Tenaya Wy Suite 122, Las Vegas, NV 89129 and serves nearby communities including Desert Shores, Sunhampton, Sun City Summerlin, Monterrey, Lone Mountain, Mar-A-Lago, and Painted Desert Estates. Whether you're looking for a dentist near me, a cosmetic dentist near me, help after a tooth extraction, or an emergency dentist who can also discuss long-term smile restoration, the process is easier when cost questions are handled upfront.
A clear path is better than guesswork
If you're comparing smile makeover options and trying to understand total cost, broad consumer pricing articles can help you frame questions before your visit. For example, this piece on the average cost of veneers per tooth is useful for understanding why personalized treatment planning matters more than one-size-fits-all pricing.
The right next step usually isn't guessing whether insurance will say yes. It's getting the teeth examined, the records gathered, and the options explained in plain language so you can make a decision with confidence.
If you're ready to find out what your plan may cover and what affordable options are available for the rest, schedule a consultation with Aspiring Smiles Dental and Braces. The team can help you review insurance benefits, discuss cosmetic and restorative choices, and build a practical treatment plan for your smile in Las Vegas.